|
The Natural Prostate Cure
Download This Book
|
Chapter 11: Testosterone Is Your Friend ________________________________________________________________________________
Nearly every medical doctor in the world will tell you that testosterone is somehow “bad” for your prostate and makes prostate cancer grow. This is unquestionable Sacred Dogma- even though the fall in testosterone as men age almost exactly parallels the rise in prostate cancer, BPH, and prostatitis. This insanity started more than eighty years ago, even before Huggins got the brilliant idea to castrate men to cure their prostate cancer! Eunuchs (castrates) had less developed sexual organs and smaller prostates, so this must have seemed like a good idea at the time. The victims seemed to get better temporarily, but the cancer soon returned with a vengeance, and they quickly died. Anyone who thinks you cure cancer by cutting off a man’s testicles is obviously insane in the first place. This butchery has continued to the present day, and now doctors use both chemicals and scalpels to castrate men.
A study from the famous Oxford University was published in the Proceedings of the Royal Society of Medicine in 1936. Testosterone was only discovered and synthesized in 1935 so it was barely known to doctors, much less available. Ironically, seventy years ago the doctors not only knew that estrogen was bad for prostate health, while testosterone was good for prostate health, they also were aware of the all important testosterone to estrogen ratio where testosterone should control and limit the “female hormone”. Over eighty studies were quoted on the entire subject.
Another study from Louisiana State University was published in the Journal of Urology in 1938. Here the doctors understood that as men aged their testosterone levels fell and the incidence of prostate disease rose greatly. Since testosterone had only been very recently discovered the patients were given fresh animal testes with good results. They referred to other studies using extracts of animal testes as well as the recently synthesized testosterone propionate. The medical profession inherently knew that “the male hormone” was good for curing BPH — a common malady even then.
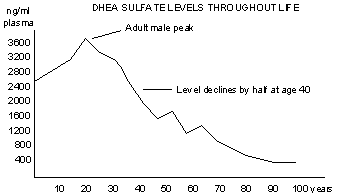
You can clearly see from this chart that testosterone levels fall as men age, while estrogen levels rise. Testosterone dominance and the testosterone-to-estrogen ratio are reversed, and prostate disease increases accordingly. Modern doctors are obviously unable to actually show studies demonstrating that testosterone causes prostate illness. Common sense tells you that testosterone is your friend, has always been your friend, and will always be your friend. as I describe in my book Testosterone Is Your Friend.
Acta Endrocnnologica 74 (1973), pp. 792—800, and 80 (1970), PP. 173—78
The scientific literature is full of countless studies that prove testosterone is necessary for good prostate health and metabolism. When blood serum testosterone levels are low, prostate receptors must choose dihydrotestosterone (DHT), which causes disease. DHT binding (not DHT blood levels) to the prostate receptors is a basic cause of illness. Let’s take just some of the many dozens of published clinical studies from around the world to prove that high, youthful levels of the androgens testosterone, androstenedione, and DHEA protect you from prostate illness, and that supplementing low testosterone and androgen levels helps you cure your illness.
At the University of Washington1 a progressive, innovative, and pioneering doctor named Richmond Prehn actually said that we should consider using androgen supplementation to reduce the growth of prostate cancer! He pointed out that declining testosterone levels contribute to carcinogenesis, and that supplementing low levels would reduce cancer rates. He pointed to earlier studies that showed low testosterone levels in prostate cancer patients indicated a much worse prognosis. It is doctors like him that are going to lead us into the medical Age of Enlightenment, and out of the Age of Darkness.
At the University of Witwaterstrand in Africa,2 a study was titled “Low Serum Testosterone Predicts a Poor Outcome in Metastatic Prostate Cancer.” They studied 122 patients and found that the ones with the HIGHEST testosterone levels had the least-aggressive tumors, and lived the longest. The patients with the lowest testosterone levels had far more aggressive growth, and died much sooner. They concluded, “Low testosterone seems to result in a more aggressive disease and a poorer prognosis in advanced prostate cancer.” This study is very clear.
At the Hubei Medical University in China,3 doctors studied men with BPH and carcinoma (PCA). They found that, “The results showed that serum testosterone in patients with BPH and PCA was lower than that of the healthy control group,” and further, “…the ratio of testosterone-to-estradiol is decreased with the rise of the age. The results suggested that the imbalance of serum sex hormones [i.e. falling testosterone and rising estrogen] was related to the pathogenesis of BPH and PCA.” It is low testosterone and high estrogen levels that cause prostate problems.
At the famous Harvard Medical School4 a study was titled “Is Low Serum Testosterone a Marker for High Grade Prostate Cancer?” They found that men with lower testosterone levels had faster growing tumors, higher Gleason scores, and shorter life spans. (Gleason scores are a measure of cancer severity.) The conclusion was, “In our study, patients with prostate cancer and a low free testosterone [level] had more extensive disease. In addition, all men with a biopsy Gleason score of 8 or greater had low serum free testosterone. This finding suggests that low serum free testosterone may be a marker for more aggressive disease.” Again, the lower the testosterone the worse the prognosis. Men, this is directly from Harvard Medical School.
At the University of Vienna,5 men with prostate cancer were compared to healthy controls. The men with cancer had decidedly lower testosterone levels than the healthy men. Again, we see that the lower the testosterone, the worse the disease and malignancy rates. They also found that the other major androgen, DHEA, did not negatively affect cancer. They said, “These data are confirmed by the present study; it can be concluded that DHEA or DHEA-S serum concentrations represent no risk factor for PC [prostate cancer] development.” This couldn’t be clearer.
Again at the University of Vienna6 men with prostate cancer were studied for their serum testosterone levels. The doctors concluded, “Low serum testosterone in men with newly diagnosed prostate cancer is associated with higher tumor micro vessel and androgen receptor density [note: both of these make the malignancies grow faster], as well as [with] higher Gleason score, suggesting enhanced malignant potential.” In other words, in men with low testosterone the tumors grew faster, the cancer was more aggressive, and the patients died sooner.
A third study from the University of Vienna7 was titled, “High Grade Prostate Cancer is Associated With Low Serum Testosterone Levels.” They found that, “patients with high Gleason score prostate cancer have lower testosterone levels.” The men with the lowest Gleason scores and slowest growing malignancies had high testosterone levels averaging 4.1 ng/ml; the ones with the highest Gleason scores and fastest growing malignancies had low testosterone levels averaging only 2.8 ng/ml. The men with almost 50% higher testosterone levels fared much better. They also found that DHEA-S levels were the same in both groups and that the powerful and beneficial androgen DHEA does not contribute to cancer, as mainstream doctors keep preaching.
Again at Harvard Medical School,8 doctors found that the cancer patients with the highest levels of testosterone fared the best and lived the longest. “A high prevalence of biopsy-detectable prostate cancer was identified in men with low total or free testosterone.” They said further, “A low serum testosterone level in men is associated with a number of medical conditions, most notably sexual dysfunction, and is commonly treated with exogenous (externally-provided) testosterone supplementation.”
At the Memphis Veterans Administration Hospital9 the good doctors found that elderly veterans fared much better when they had higher testosterone levels. “Patients with a pretreatment testosterone level of less than 300 ng/100 ml had shorter intervals free of progression than patients with pretreatment testosterone levels of greater than 300 ng/100 ml.” They referred to studies as early as 1971 that showed the same previous phenomenon. The higher the testosterone levels the longer the men lived; the lower the levels the earlier they died.
In an impressive collective effort between six international clinics,10 including UCLA and Columbia University, scientists used the Norwegian Cancer Registry to study the frozen blood serum and medical records of approximately 28,000 men. The median age of the men at blood draw was sixty years old. They found that the healthy men actually had higher testosterone levels than the ones who developed prostate cancer. They concluded that the idea of testosterone increasing the risk of prostate cancer is completely unsupported in any way. Men, this study is the second largest ever done on testosterone and prostate cancer. You just can’t argue with its conclusions based on 28,000 real men.
The University of Chicago and three other clinics11 found the exact same results. “A separate analysis of serum testosterone levels revealed that the higher the pretreatment serum testosterone level, the greater the survival rate. Compared with patients with serum testosterone levels of less than 6.9 nmo/L, significant differences in survival were observed for patients with serum testosterone levels of 10.4 to 13.9, 13.9 to 17.3, and those higher than 17.3 nmo/L.” This means that the higher the testosterone levels were, the longer the men lived and the better they fared. “These results have important implications for the design and analysis of future clinical trials of hormone therapy.” Doctors should be giving men testosterone therapy, rather than “androgen ablation.” They actually came out and said this in plain words.
At the famous Johns Hopkins University in Baltimore12 more men were studied. One group was healthy, one had BPH, and one had prostate cancer. Their total testosterone (measured in ng/dl) was measured over a five-year period. The healthy men had an average level of 636.1, the BPH group only 527.4, the men with localized cancer averaged 472.6, and those with metastatic cancer 567.7. Clearly, the healthy men had much higher levels of testosterone. Strangely enough, the conclusion was, “These data suggest that there are no measurable differences in serum testosterone levels among men who are destined to develop prostate cancer and those without the disease”!!! These doctors simply did not want to admit that low testosterone was found in the BPH, low cancer, and metastasized cancer patients. A dramatic difference of 35 percent certainly should have proved the case decisively. They actually tried to deny their own results.
At the University of Utah13 researchers did a unique study in which they compared 214 sets of male twins. Using identical twins is a most effective means to demonstrate scientific validity. They found that the higher the testosterone levels, the smaller prostate glands were. “Prostate volumes correlated inversely with age-adjusted serum testosterone.” The men with the smallest prostates had testosterone levels of 17.7 / 7.9 / 17.9 nmo/L, while the men with the largest glands had levels of only 14.7 / 6.0 / 14.2. To prevent or cure BPH, a man certainly wants to maintain a youthful testosterone level. Any man over the age of 40 should know his free testosterone level, and supplement it as necessary.
At the Petrov Institute of Oncology in Russia,14 men (average age about 40) were divided into two groups of high and low blood testosterone. The first group was given 120 mg daily of oral testosterone undecanoate, and the second 80 mg. Their prostates were reduced in volume, generally in six months. “These findings suggest that exogenous testosterone in middle-aged and older men with some clinical features of age-related androgen deficiency can retard or reverse prostate growth.” Everyone knows that the gradual decrease in male testosterone levels after the age of about thirty clearly coincides with the abnormal increase in prostate volumes (BPH). The need for testosterone supplementation is obvious, yet doctors somehow can’t see this. Using oral testosterone salts was a very bad idea, the doses were too high, and they would have gotten far better results with natural transdermal or sublingual testosterone delivering about 3 mg a day.
At the famous Tenovus Institute in Wales15 over two hundred prostate cancer patients were studied. Again they found that the men with the lowest testosterone levels had the poorest prognosis and died the soonest. “Low concentrations of testosterone in plasma at the time of diagnosis related to a poor prognosis. Patients who died within one year of diagnosis had the lowest mean plasma levels of this steroid.” They went on to repeat, “The results of this study suggest that low plasma testosterone concentrations in men with prostatic carcinoma at the time of initial diagnosis is associated with a poor prognosis. The highest levels of plasma testosterone were found in those patients who subsequently survived the longest.” This study was done almost twenty years ago and was published in a major journal. Why are doctors still castrating men with knives and toxic chemicals to destroy their testosterone?
At the University of Connecticut16 doctors gave elderly, hypogonadal (low testosterone) men either transdermal testosterone (the natural and correct way) or injections of testosterone salts (the unnatural and wrong way), for several months. They found, “There were no ill effects on prostate size, symptoms, or prostate specific antigen [PSA] level.” If they had measured more health parameters they would have found that the men responded well overall, and got many benefits from raising their testosterone. If testosterone has negative effects (as 99.9 percent of the world’s doctors believe), then they would have enlarged their prostates, raised their PSAs, and gotten high rates of cancer- since basically all men over seventy already have growing cancer cells in their prostates. These sacred beliefs were further disproved with the low-testosterone (hypogonadal), elderly men who were given supplemental testosterone. The doctors reiterated, “No significant side effects in prostate tests or symptoms were seen in this study.”
A similar study was done at the Brooke Army Medical Center in Texas17 where older men were given injections of supplemental testosterone salts for six months. The doctors concluded, “Parenteral [injection] testosterone replacement in hypogonadal men with normal pretreatment digital rectal examination and serum PSA levels does not alter PSA or PSA velocity beyond established non-treatment norms.” If testosterone causes prostate problems, obviously their PSA levels would have gone up dramatically. The doctors should have used natural transdermal or sublingual testosterone, but still the men generally benefited from the therapy.
A quarter of a century ago at the Granada Medical Facility,18 men with BPH were studied and compared with healthy men of the same age group. They found that the men with BPH had a 43% lower testosterone level than the normal men. The men with BPH had an average level of only 2.3 ng/ml, while the healthy men’s levels averaged 4.0 ng/ml. Obviously 43 percent is a very dramatic difference and proves again that low testosterone causes prostate disease. “The testosterone concentration in the BPH group was significantly lower than that of the healthy control group.” The authors were also well aware that estradiol rises strongly in men as they age, and that estradiol supplementation causes abnormal growth in the prostate gland. All this twenty-five years ago in a major journal, yet ignored today.
At the Royal London Hospital19 doctors did a stunning review of thirty-four studies, complete with fifty-five references, and revealed that the Huggins testosterone “dogma” has been completely unsupported by science for the last sixty years. “Yet there has so far been no conclusive evidence, despite thirty-four studies, that levels of circulating testosterone in individuals developing prostate cancer are higher than in controls.” They quoted other studies: “Three overviews provided similar evidence that there is no significant difference in mean testosterone levels between patients and control.” They went on to say, “Firstly, prostate cancers arising in men with low serum testosterone levels are more malignant and frequently unresponsive to hormones [e.g. estrogen].”
At the National Cancer Institute in Maryland20 men with prostate cancer were studied and compared to healthy controls. On the surface, the testosterone levels appeared the same. However, the testosterone-to-estradiol ratios in healthy men were higher, at 7.00, compared to 6.68 in the cancer patients (higher is good, since testosterone should dominate estradiol.) The testosterone-to-estradiol ratio is just as important as the actual free testosterone level itself. As men age, their testosterone levels fall and their estrogen levels actually become higher than women of the same age(!), since estrogen, instead of testosterone, becomes dominant.
At the Beth Israel Hospital in New York City21 researchers studied men for thirteen different hormones (or their metabolites) to determine which ones contributed to the growth of their carcinomas. They found that the average cancer patient had a low testosterone level of about 350 ng/dl, compared to the healthy controls’ much higher levels of about 450 ng/dl. In the men under sixty-five, the difference was much more dramatic, with levels of 282 ng in cancer patients compared to 434 ng for the healthy controls — over 50 percent higher testosterone in healthy men without cancer. The researchers were very reluctant to admit what they found. They also found that the cancer patients had much lower DHEA levels as well. The estrone levels were also clearly “markedly higher” in cancer patients. More proof that it is estrogens, and not the androgens DHEA and testosterone, that cause malignancy.
The internationally renowned Karolinska Institute in Sweden22 studied 2,400 cancer patients and found that the prostate cancer patients had 8 percent lower testosterone than healthy controls. Prostate cancer is the leading cause of male cancer deaths in Sweden, mainly due to high-fat diets. The conclusion was, “Testosterone levels were lower in patients with cancer than in controls.” Again, we see that high, youthful testosterone levels help prevent cancer.
Again at the University of Utah, the same doctors23 studied the brothers of men with prostate cancer and found they had four times the chance of also getting cancer. They found that the high-risk brothers had much lower testosterone levels than healthy controls. “The observation of a lower rather than higher plasma testosterone content in men at risk for the cancer might indicate that tissue responsiveness is supranormal.” They also found a much lower testosterone-to-estradiol ratio, which demonstrated estrogen dominance, with rising estradiol and falling testosterone. The controls had a desirable 162.5:1 ratio, while cancer patients had only a 132.5 ratio. This ratio is just as important as the free testosterone level itself.
Twenty years ago, at the University of Helsinki24 hormones were measured in men with BPH or prostate cancer, against healthy controls. The free testosterone levels of the BPH patients averaged only 301 pmol/L, the cancer patients just 249 pmol/L, while the healthy men had a high 380 level. The healthy men had low estradiol levels of only 53.5 pmol/L, while the BPH patients had a stunning 137.4 pmol/L, and the cancer patients 83.7. The healthy men had testosterone-to-estradiol ratios of 7.1:1 (high is good), while the BPH men had 2.2, and the cancer patients only 3.0. The poor doctors still couldn’t figure out that excess estrogens cause prostate disease, while high, youthful testosterone levels prevent and cure it. Fifty years ago (a half-century!) at Boston University25 doctors studied men on testosterone therapy to see what effect it had on their prostate glands. These subjects had used testosterone propionate (doctors really didn’t know any better at the time, and transdermal creams were unknown) for four years. Healthy controls of the same age were compared. The men who were on testosterone therapy had less palpable irregularities and less hypertrophy than the healthy controls. Even using the wrong kind of testosterone resulted in better prostate health, fewer irregularities, and less BPH. They concluded, “In this study, there was no evidence that testosterone propionate in the dosage used had initiated carcinoma or activated latent carcinoma of the prostate gland.” Actually, they found less prostate disease of all kinds in testosterone-supplemented men.
At the National Public Health Institute in Finland, 26 doctors based their study on 62,440 Finnish men to see if testosterone and its precursor, androstenedione, increased prostate cancer rates. They concluded, “There was no association [detected] between serum testosterone or androstenedione concentrations and the occurrence of subsequent prostate carcinoma in the total study population or in subgroups, based on age [or] body mass index [BMI].” The actual numbers showed that healthy men had 11% higher androstenedione than the cancer patients. They further said, “The results of the current study do not appear to corroborate the hypothesis that serum testosterone or androstenedione are causes of the subsequent occurrence of prostate carcinoma.” This is the largest study on record based on 62,440 men.
At the International Agency for Research on Cancer, in France,27 doctors did a very impressive review of the literature, complete with two-hundred forty-seven citations. Twenty-two major studies from around the world were analyzed in great detail. They came right out and said, ‘”A first conclusion of this review is that, taken together, epidemiological studies have provided little support for the hypothesis that prostate cancer risk is increased in men with elevated total or bio-available testosterone.” They did, however, find that elevated IGF-1 (insulin-like growth factor) levels were clearly correlated with prostate disease. A review of twenty-two other studies proves testosterone is good for prostate health.
At Umea University Hospital in Sweden28 almost 3,000 men both with and without prostate cancer were studied for their blood androgen levels. The men with the highest levels of testosterone had the least rates of cancer, while the men with the lowest levels of testosterone had the highest rates of cancer. The doctors were stunned at the results since they clearly started out to prove, “androgens stimulate prostate cancer in vivo and in vitro.” They began with a bias against testosterone and had to reverse themselves due to their own findings.
Again, at Harvard Medical School29 doctors really took a big risk in going against the prevailing negative view of testosterone and prostate health. They took 75 men with low testosterone, 20 of whom had a precancerous condition called “prostatic intraepithel- ial neoplasia” or PIN. They gave all of these men supplemental testosterone for one year knowing that the prevailing medical opinion is that the twenty men with PIN should be expected to get outright cancer of the prostate. Of course nothing of the sort happened. The men were in much better mental and physical health after raising their testosterone levels to normal ones and their prostate glands prospered having the testosterone they needed. Give these doctors a lot of credit here for courage.
At Taipei Veterans Hospital30 ninety-six men with advanced metastatic prostate cancer were studied for their hormone levels including testosterone, LH, FSH and prolactin. They were divided into two groups based on their testosterone levels. Group 1 had 77 percent higher testosterone levels than group 2. Group 1, who fared the best, had the highest testosterone levels. Group 2, the ones whose cancer grew quickly, had the lowest testosterone levels. The doctors concluded, “Higher testosterone and lower LH, FSH and prolactin levels were good prognostic factors for patients with metastatic prostate cancer undergoing hormonal treatment, irrespective of tumor grading.” These doctors still insisted on using hormonal ablation “therapy” to destroy their testosterone to castrate levels. Incredible!
Over a quarter century ago at the famous Tenovus Institute for Cancer Research in Wales31 doctors found out that low testosterone was clearly correlated with both BPH and prostate cancer. They actually tried to deny this fact, in spite of the blood tests they had! This proves the medical profession is more interested in keeping the status quo than finding the truth. The healthy men had 17 percent higher testosterone levels than the men with prostate cancer, yet they tried to claim these levels ”were not significantly different.” 17 percent is very statistically significant in any study obviously. The men with BPH also had significantly lower testosterone levels. Of course they still poisoned these poor men with stilbestrol (a synthetic estrogen) to destroy all testosterone production and make them worse.
At Yamagata University in Japan32 a first rate study was done with men suffering from BPH compared to healthy controls. The men with BPH had 19 percent larger prostates and a stunning 390 percent higher estradiol levels. The healthy men had 49 percent higher free testosterone levels and 46 percent higher total testosterone levels. The healthy men had an excellent .99 testosterone to estrogen ratio, while the diseased men had a terrible .17 testosterone to estrogen ratio. Again, the authors actually tried to deny the testosterone levels were related to prostate volume since this contradicted the accepted medical dogma! Truth just doesn’t interest them.
Way back in 1981 at the University of Helsinki in Finland 33 doctors studied the hormonal profiles of men with prostate cancer. The men who lived longest had a full 33 percent higher testosterone (T) level and an impressive 67 percent higher progesterone level. The men who died the earliest had 33 percent higher estradiol and 36 percent higher estrone. The men who fared the best had a 1.1 T to E2 ratio and a 0.3 T to E1 ratio, while the sickly men had a poor 0.6 T to E2 ratio and a 0.2 T to E1 ratio. They concluded, “The statistical findings that patients with higher plasma T and lower oestrogens (the English spelling) have a good response to treatment also have a logical basis in the available literature.” Further they said, “In patients with a good response, the mean plasma T level was significantly higher than in patients with poor response.”
At the Harvard School of Public Health and other clinics34 men (average age seventy-two) with prostate cancer were compared to healthy men. The healthy controls had a full 21 percent higher levels (average 541.8 ng/ml) of testosterone (T) than the cancer patients (average 447.1 ng/ml). The authors again tried in vain to deny that low testosterone was clearly correlated with prostate cancer despite the results. This is a very powerful human “case control study” headed by the famous Harvard University. When supposed scientists are so biased as to try to deny their own data, this shows the entrenched dogma in the medical profession is more interested in dogma and tradition than truth and facts. They actually tried to say that, “T was associated marginally positively” to infer exactly the opposite of what they found.
At Helsinki University in Finland35 one hundred and twenty-three men (average age of seventy-two) with prostate cancer were studied for their hormone levels. “Low pretreatment values (of testosterone) indicated poorer prognosis”, was their conclusion. The lower the free testosterone level, the higher the Gleason score. The lower the free testosterone the more aggressive and faster growing were the tumors. The lower the free testosterone the more the cancer metasticized. After four years 80 percent of the men with the higher testosterone levels were still alive, but only 45 percent of the men with the lower testosterone levels were still alive. Only 20 percent dead vs. a full 55 percent dead. High testosterone wins again.
At the Munich University Clinic36 a case control study was done on actual prostate tissue in healthy men and men with BPH. They found, “The mean levels of estradiol and estrone were significantly higher in BPH.” The further said, “Our results indicate that the prostatic accumulation of DHT, estradiol and estrone is in part intimately correlated with aging, leading with increasing age to a dramatic increase of the estrogen/androgen ratio particularly in stroma of BPH.” They found low-prostate stroma tissue levels of testosterone of course. Binding of DHT and estrogens causes BPH, while binding of testosterone is protective.
Men, we can go on with studies like these all day. At the University of North Carolina37 healthy men were compared to men with outright prostate cancer. The healthy men had 22% higher testosterone levels. At the University of Iowa 38 healthy men were injected with completely irresponsible amounts of testosterone salts up to 500 mg weekly. “No significant change occurred in the prostate volume or serum PSA levels at any dose of exogenous testosterone.” Again, at the University of Iowa39 men were injected with ridiculous amounts of testosterone salts up to 500 mg yet, “Serum PSA is not responsive to elevated serum testosterone levels.” At the Hamburg University Clinic in Germany40, men were studied for their hormone levels. The healthy men had higher testosterone levels, while the men with BPH and cancer had lower levels. At Harvard Medical School41 researchers found that men with BPH had lower testosterone and androstenedione levels than healthy men, and that estrogen dominance over testosterone, as men aged, was a clear cause of hypertrophy. At the famous Walter Reed Army Medical Center in Washington,42 hypogonadal men got either testosterone enanthate injections or transdermal testosterone. They concluded, “This study suggests that in hypogonadal men neither PSMA [membrane antigen] nor PSA expression is testosterone dependent.” At the Moscow Medical Institute,43 they clearly found that, “In normal men over sixty years old, the plasma levels of FSH [follicle-stimulating hormone] and estradiol were higher, and those of prolactin, testosterone, and estriol [the “safe” estrogen] were lower than those of normal men.” In mainland China44 doctors found, “The serum level of testosterone was less and that of prolactin was greater in BPH [men] than in normal subjects.” At Adis International Ltd, in New Zealand45 researchers gave transdermal testosterone to hypogonadal men for a whole year. This normalized their testosterone-to-estrogen ratios, improved their erectile response, and made their overall sexual function better. “PSA levels and prostate volumes remained in the normal range during long-term treatment.” At Queen’s University in Canada,46 they did a review of the literature and said, “The current evidence does not support the view that appropriate treatment of elderly hypogonadal men with androgens has a causal relationship with prostate cancer.” At the Institute of Reproductive Medicine in Germany47 men were treated with transdermal testosterone for up to TEN years, and “prostate specific antigen levels were constantly low in all patients.” At the University of California at Los Angeles,48 racial groups of men averaging seventy years of age were studied. The Asian men with the highest levels of free testosterone had the lowest rates of prostate disease. Caucasians with the lowest levels of free testosterone had the highest rates of prostate disease. At the Imperial Cancer Research Fund in London49 men were studied for their hormone levels. The healthy men had higher plasma testosterone levels than the men with prostate cancer, and much higher levels than the men with advanced metastatic cancer. At the University of Medical Science in mainland China50 Chinese men were studied for their serum testosterone levels. The healthy men had higher levels than the BPH or cancer patients.
At the University of California at Davis51 cancer patients were studied and the doctors said, “Men with prostate carcinoma and low testosterone levels have a much worse prognosis. At Nijmegen University Hospital in the Netherlands52 doctors said, “Low testosterone concentration at the start of therapy was also associated with poor prognosis.” At Johns Hopkins University53 again, men with prostate cancer had decidedly lower DHEA and DHEA-S levels than healthy controls. At the Akademy of Medizin in Poland54 men with BPH had lower levels of testosterone than the healthy controls they were matched with. At the Veterans’ Administration Center in Los Angeles55 doctors admitted that they got no benefit from androgen ablation, no matter if the testosterone was literally lowered to zero. At the American Health Foundation in New York56 black men with prostate cancer were compared to healthy black men. The cancer patients had lower testosterone, androstenedione, and DHEA, while they also had higher estrone and estradiol levels. A very long study was done at the University of Copenhagen lasting almost five years57 using two-hundred forty-five men with prostate cancer. The men with the highest levels of testosterone lived the longest by far with the highest quality of life and slowest growth of cancer. The men with the lowest levels died sooner and had a much lower quality of life with faster growing malignancies. “Pretreatment level of serum testosterone was confirmed as having significant prognostic value on progression-free, overall and cancer-specific survival.” At the Royal Postgraduate Medical School in London58 thirty years ago men with BPH were compared with healthy controls. The healthy men with an average 475 ng/ml had a significant 8% higher testosterone level than the diseased patients with an average 438 ng/ml level. Again, the authors tried to deny there was any difference as the results didn’t fit in with their preconceptions! German doctors59 injected testosterone salts into hypogonadal men for over three years. Even though this is the wrong way to raise testosterone, the prostate volume did not increase, the PSA did not rise and there was no increase in rates of prostate disease of any kind. Quite the contrary, men got dramatic benefits in many ways. At the University of California in Torrance60 doctors gave natural testosterone transdermal gel to hypogonadal men for three years. The men got dramatic benefits and, “Levels of PSA…. remained in the normal range.” At the University of Utah61 doctors gave hypogonadal men both injections and transdermal patches of testosterone and found, “Prostate size during therapy was comparable to that reported for normal men. In these men treated with transdermal testosterone, PSA levels were also within the normal range.”
At the University of Iowa62 110 men with prostate cancer were studied. Clearly the higher their testosterone the slower the tumor growth and the longer they lived. “Patients with a pretreatment testosterone level of less than 300 ng/100 ml…. had the most rapid progression.” Over a quarter century ago doctors at the National Cancer Institute63 compared healthy men to ones suffering from BPH. The healthy men had an average full 146 percent higher testosterone level than the afflicted men. At Roswell Institute in NY64 normal men were compared to those with BPH. The healthy men had 152 percent more testosterone on the average than the patients. This was also a quarter century ago and is hardly news. At the University of TN65 the longevity of men with prostate cancer higher testosterone was “the most significant variable” of all parameters studied in the longest-lived patients. At the Karolinska Institute hypogonadal men were given testosterone patches for a year. Their PSA stayed the same as did their prostate volume as determined by ultrasound66. At Beth Israel Center67 an review of seventy-two studies showed there was, “no causal relationship between testosterone and prostate cancer risk.” At the Cross Cancer Institute in Canada68 it was found that the men with the lowest testosterone levels died the soonest and their cancer grew the fastest. That’s sixty-eight published studies to prove the point. Every month another one is published.
References 1. Cancer Research 59 (1999), pp. 4161-64 2. American J. Clinical Oncology 20 (1997, pp. 605-08 3. Hubei Yike Daxue Xuebao 19 (1998), pp. 241-42 4. Journal of Urology 163 (2000), pp. 824-27 5. Prostate 44 (2000), pp. 219-24 6. Journal of Urology 169 (2003), pp. 1312-15 7. Prostate 47 (2001), pp. 52-58 8. Journal of the American Medical Assoc. 276 (1996), pp. 1904-06 9. Journal of Urology 144 (1989), pp. 1139--42 10. Cancer Epidem., Biomarkers & Preview 6 (1997), pp. 967-69 11. Journal of the American Medical Assoc. 265 (1991), pp. 618-21 12. Prostate 27 (1995), pp. 25-31 13. Journal Clinical Endocrin. Med. 82 (1997), pp. 571-75 14. International Journal of Andrology 25 (2002), pp. 119-25 15. European Journal of Cancer 20 (1984), pp.477-82 16. Endocrine Research 26 (2000), pp. 153-68 17. Journal of Urology 158 (1997), pp. 1775-77 18. Experientia 35 (1978), pp. 844-45 19. Drugs and Aging 17 (2000), pp. 431-39 20. Cancer Epidemiology Biomarkers & Preview 2 (1993), pp. 27--32 21. Prostate 3 (1982), pp. 579--88 22. British Journal of Urology 77 (1996), pp. 433--40 23. Prostate 6 (1985), pp. 121-28; and Journal of Clinical Endocrinology & Metabolism 54 (1982), pp. 1104-08 24. Prostate 4 (1983), pp. 223-29 25. Journal of Clinical Endoc. & Metabolism 15 (1954), pp. 297--30 26. Cancer 86 (1999), pp. 312-15 27. Prostate Cancer 3 (2000), pp. 157-72 28. Int. J. Cancer 108 (2003) pp. 418-24 29. Journal of Urology 170 (2003) pp. 2348-51 30. BJU Inter. 89 (2002) pp. 710-13 31. Acta Endoc. 81 (1976) pp. 409-26 32. J. Androl. 21 (2000) pp. 258-61 33. Acta Endoc. 98 (1981) pp. 634-40 34. Cancer Causes and Controls 8 (1997) pp. 632-6 35. Prostate 12 (1988) pp. 325-32 36. J. Clin. Endoc. Metab. 77 (1993) pp. 375-81 37. Prostate 11 (1987) pp. 171-82 38. J. Urol. 159 (1998) p. 441-3 39. J. Urol 156 (1996) pp. 438-42 40. Acta Endocrinologica 90 (1979), pp. 77-36 41. Prostate 26 (1995), pp. 40-49 42. Journal of Surgical Oncology 59 (1995), pp. 246-50 43. Akad. Med. Nauk SSSR 3 (1980), 72-77 44. Zhonghua Yixue Zazhi 73 (1993), pp. 489-90 45. Drugs 55(1998), pp. 253-58 46. European Urology 41 (2002), pp. 113-20 47. Clinical Endocrinology 50 (1999), pp. 629-35 48. Cancer Epidimiology Biomarkers & Preview 4 (1995), pp.735-41 49. British Journal of Medicine 4 (1971), pp. 391-94 50. Hejishu 16 (1993), pp. 649-52 51. Cancer 83 (1998), pp.1170-73 52. Cancer 65 (1990), pp. 2758-61 53. Cancer Epidemiology Biomarkers & Preven. 2 (1993), pp. 219-21 54. Akad. Med. Bialymstoku Supp. 42 (1984), p. 17 55. Journal of Urology 99 (1968), p. 788-92 56. Cancer Research 42 (1982), pp. 3864-69 57. Scand. J. Urol. Nephrol. 157 (1994) pp. 41-7 58. British Journal of Urology 49 (1977) pp. 541-4 59. Journal of Andrology 23 (2002) pp. 419-25 60. Aging Male 6 (2003) pp.207-11 61. Urology 49 (1997) pp. 191-6 62. Journal of Urology 141 (1989) pp. 1139-42 63. Surgical Forum 28 (1977) pp. 568-9 64. Oncology 37 (1980) pp. 46-52 65. Urology 33 Supp. (1989) pp. 53-6 66. Journal of Urology 155 (1996) pp. 1604-8 67. New England Journal of Medicine 350 (2004) pp.482-92 68. Journal of Urology 146 (1991) pp. 372-6
|